Geocoding for Healthcare: Patient Mapping, Facility Planning & HIPAA Compliance
How hospitals and health systems geocode patient addresses for access analysis, facility planning, CHNA reporting, and outbreak detection. Free batch geocoding with HIPAA compliance.
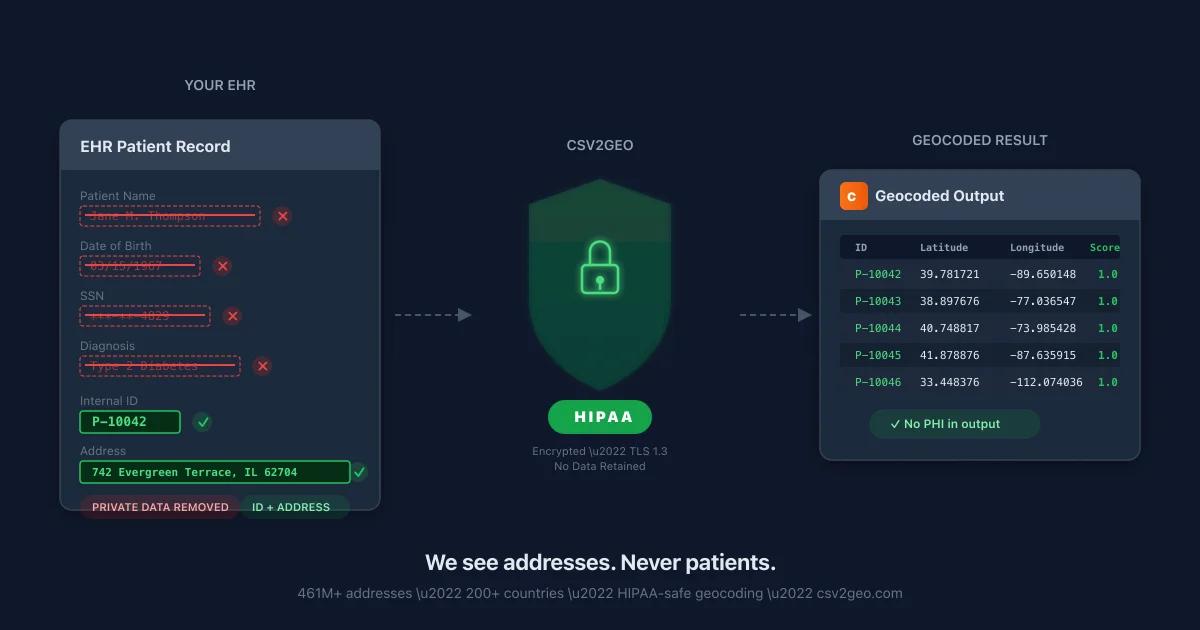
A community health center in rural Appalachia serves 14 counties across three states. Their patient records contain 23,000 home addresses. The director needs to answer a question that determines next year’s $2.4 million federal grant renewal: How many patients live more than 30 miles from the nearest clinic?
Without geocoding, answering this question means someone opening Google Maps 23,000 times. With a batch geocoding tool, the answer takes four minutes. Upload a CSV of patient addresses, get latitude and longitude coordinates back, calculate distances to clinic locations, and generate a map that satisfies the grant reviewer on slide one.
This guide breaks down how healthcare organizations actually use geocoding for patient mapping, facility planning, health equity analysis, and community outreach — without violating HIPAA.
What Geocoding Does for Healthcare Organizations
At its core, geocoding converts a street address into latitude and longitude. For healthcare, that means turning the home address sitting in your EHR — plain text, basically useless for spatial analysis — into a point on a map you can measure against anything.
With coordinates, you stop guessing and start measuring. How far does each patient actually travel to reach your facility? Which ZIP codes cluster the highest diabetes prevalence? Where should the next urgent care clinic go to shave 15 minutes off average patient drive time? Which neighborhoods hit the ED three times more than the county average — and could a mobile unit cut that in half?
Population health management, network adequacy filings, CHNAs, disease surveillance — all of these live or die on knowing where patients are in geographic space. An address in a database is a string. A geocoded address is actionable intelligence.
6 Healthcare Use Cases for Geocoding
Patient Access Analysis
Measure drive times and distances between patient homes and facilities. Identify access deserts where patients travel 45+ minutes for care.
Facility Site Selection
Map patient density by neighborhood to determine optimal locations for new clinics, urgent care centers, or mobile health units.
Community Health Needs Assessment
Overlay patient data with census demographics, social determinants, and disease prevalence by geography for CHNA reporting.
Emergency Preparedness
Map medically fragile patients by location before a hurricane, wildfire, or flood to prioritize evacuation outreach.
Disease Surveillance
Plot confirmed cases by coordinates to identify outbreak clusters, track disease spread, and allocate public health resources.
Patient Outreach Campaigns
Target preventive care reminders, vaccination drives, and screening campaigns to specific geographic areas based on patient distribution.
1. Patient Access and Drive-Time Analysis
CMS (Centers for Medicare & Medicaid Services) requires Medicare Advantage plans to demonstrate network adequacy — meaning patients must be able to reach specific provider types within defined time and distance standards. For urban areas, a primary care provider must be within 10 miles or 15 minutes. For rural areas, the standard expands to 60 miles or 75 minutes.
To prove network adequacy, health plans geocode every member address and every contracted provider address, then calculate pairwise distances. A plan with 200,000 members and 5,000 providers generates one billion distance pairs. Without geocoded coordinates, this calculation is impossible.
| CMS Network Adequacy Standard | Urban | Suburban | Rural |
|---|---|---|---|
| Primary care | 10 mi / 15 min | 25 mi / 30 min | 60 mi / 75 min |
| Specialist (cardiology, oncology) | 15 mi / 20 min | 35 mi / 40 min | 75 mi / 90 min |
| Hospital (acute inpatient) | 15 mi / 20 min | 30 mi / 35 min | 60 mi / 75 min |
| Behavioral health | 10 mi / 15 min | 25 mi / 30 min | 60 mi / 75 min |
| Pharmacy | 5 mi / 10 min | 15 mi / 20 min | 30 mi / 40 min |
In practice, you pull member addresses from your enrollment system into a CSV, run them through a geocoding service, and get coordinates back. Then you calculate haversine distances (straight-line) or hit a routing API for actual drive times. Any member outside the distance standard is a gap — and CMS will flag it on review.
2. Facility Site Selection
A hospital system planning a new ambulatory surgery center does not pick a location by intuition. They geocode their surgical patient addresses from the past three years, generate a heat map of patient density, identify the geographic centroid of demand, then evaluate available real estate within that zone.
The same approach works for urgent care clinics, dialysis centers, behavioral health offices, and mobile health unit routes. Geocode your patients, map them, and let the data tell you where the demand is densest and the supply is thinnest.
A practical example: A health system in Phoenix geocoded 45,000 patient addresses and discovered that 8,200 patients in the northeast corridor were driving past two competitor facilities to reach their hospital 22 miles south. This single insight justified a $12 million ambulatory center investment that captured those patients closer to home.
3. Community Health Needs Assessment (CHNA)
IRS requires every non-profit hospital to conduct a Community Health Needs Assessment every three years. A CHNA identifies the most pressing health needs in the community the hospital serves. Geocoding is the backbone of every modern CHNA.
The mechanics are straightforward: geocode your patient population, then overlay with Census Bureau data — poverty rates, uninsured rates, educational attainment, language barriers — all available at the census tract level. Layer in public health data: diabetes prevalence, opioid overdose rates, maternal mortality, food desert classifications. What comes out is a geographic profile of community health needs that is specific enough to drive funding decisions and defensible enough to survive a board presentation.
| CHNA Data Layer | Source | Why Geocoding Is Required |
|---|---|---|
| Patient distribution | Your EHR/billing system | Addresses must be converted to coordinates for spatial analysis |
| Poverty rate by tract | Census ACS (S1701) | Census data is indexed by tract FIPS code, matched via coordinates |
| Uninsured rate | Census ACS (S2701) | Same — requires coordinate-to-tract lookup |
| Medically underserved areas | HRSA MUA/MUP database | MUA boundaries are geographic polygons |
| Food deserts | USDA Food Access Research Atlas | Defined by census tract, matched by coordinates |
| Life expectancy | CDC PLACES / USALEEP | Available at census tract level, joined by geography |
| Opioid overdose rates | CDC WONDER | County-level data, mapped via geocoded coordinates |
Without geocoding, a CHNA is a collection of county-level averages that mask neighborhood-level disparities. With geocoding, you can show that Block Group 3 in Census Tract 1042 has a 34% poverty rate, a 22% uninsured rate, and zero primary care providers within 10 miles — the kind of specificity that drives targeted intervention and earns grant funding.
4. Emergency Preparedness and Disaster Response
When Hurricane Ian hit Southwest Florida in 2022, hospitals needed to identify which patients required immediate outreach: dialysis patients, ventilator-dependent patients, patients on refrigerated medications. The ones who had geocoded patient registries could overlay patient coordinates with the storm surge map within hours. The ones who had not were making phone calls to every patient in a five-county area.
The whole trick is doing the geocoding before the storm, not during it. Pre-geocode your high-risk patient populations and keep the file updated quarterly. When something hits, you already have coordinates — you just overlay them on the hazard map.
- Export addresses of medically fragile patients (oxygen, dialysis, insulin, home health) from your EHR
- Batch geocode all addresses — get coordinates for each patient
- Store the geocoded file securely (coordinates do not change when storms do)
- When a disaster threatens, overlay patient coordinates with the hazard zone (hurricane cone, flood map, wildfire perimeter)
- Generate a prioritized contact list: patients inside the hazard zone, sorted by medical acuity
This five-step process, completed before hurricane season, turns a 72-hour scramble into a 30-minute GIS query.
5. Disease Surveillance and Outbreak Detection
John Snow mapped cholera cases on a London street map in 1854 and found the contaminated pump. The method has not changed — the speed has. A county health department pulling 500 COVID test results daily can geocode every one of them in seconds, plot them, and catch a cluster forming at a specific apartment complex before the local news does.
Where this matters most:
- Cluster detection: identifying statistically significant geographic concentrations of disease
- Contact tracing: mapping confirmed cases to identify potential exposure locations
- Resource allocation: directing testing sites, vaccination clinics, and outreach workers to the areas with highest case density
- Disparity analysis: comparing case rates between neighborhoods to identify disproportionately affected communities
The CDC’s National Notifiable Diseases Surveillance System (NNDSS) relies on geocoded case data for national-level disease mapping. State and local health departments feed this system — and geocoding is how addresses become mappable data points.
6. Patient Outreach and Preventive Care Campaigns
A federally qualified health center (FQHC) in Houston wants to increase colorectal cancer screening rates among patients aged 45-75 who are overdue. They export 6,200 patient addresses from their EHR, geocode them, and discover that 2,100 patients cluster within three ZIP codes on the east side of the city. Instead of mailing 6,200 letters, they deploy a mobile screening unit to those three ZIP codes and run a targeted phone campaign. The result: 3x higher screening completion rate at 40% of the cost.
This pattern — geocode, cluster, target — works for flu vaccination drives, diabetes management outreach, well-child visit reminders, prenatal care enrollment, and any other preventive service where geographic targeting beats blanket outreach. If you are working with large files of 100K+ addresses, the same workflow scales without changing the approach.
How to Geocode Patient Addresses (Step by Step)
Step 1: Export Addresses from Your EHR
Most electronic health record systems (Epic, Cerner, Athena, eClinicalWorks) allow you to export patient demographics as a CSV or Excel file. You need, at minimum, the street address, city, state, and ZIP code. A typical export looks like this:
| Patient ID | Street | City | State | ZIP |
|---|---|---|---|---|
| P-10042 | 742 Evergreen Terrace | Springfield | IL | 62704 |
| P-10043 | 1600 Pennsylvania Ave NW | Washington | DC | 20500 |
| P-10044 | 350 Fifth Avenue | New York | NY | 10118 |
| P-10045 | 233 S Wacker Dr | Chicago | IL | 60606 |
Important: Do not include patient names, dates of birth, Social Security numbers, or any other Protected Health Information (PHI) beyond the address. The address itself is PHI under HIPAA, but it is the minimum required for geocoding. Strip everything else before uploading.
Step 2: Upload to a Geocoding Service
Drag your CSV onto the batch geocoding upload page. The system auto-detects your columns — confirm the street, city, state, and ZIP mappings if prompted, then hit Process. For 10,000 patient addresses, you are looking at roughly 15 seconds.
Nothing persists on the server after you download. The addresses are processed, coordinates are returned, and the temporary files are wiped. No patient addresses get retained, logged, or shared with anyone.
Step 3: Download the Geocoded File
The output file adds latitude, longitude, and a confidence score to each row. A confidence score of 1.0 means the address matched at the rooftop level — the exact building. A score below 0.5 means the geocoder could only match to a city or ZIP centroid, which may indicate a bad address.
| Patient ID | Latitude | Longitude | Confidence | Match Level |
|---|---|---|---|---|
| P-10042 | 39.781721 | -89.650148 | 1.0 | Rooftop |
| P-10043 | 38.897676 | -77.036547 | 1.0 | Rooftop |
| P-10044 | 40.748817 | -73.985428 | 1.0 | Rooftop |
| P-10045 | 41.878876 | -87.635915 | 1.0 | Rooftop |
Step 4: Analyze in Your Tool of Choice
With coordinates in hand, open the file in any GIS or analytics tool:
- QGIS (free, open source) — create heat maps, calculate distances, overlay with census data
- ArcGIS Online — enterprise mapping with HIPAA-compliant hosting options
- Tableau or Power BI — interactive dashboards with geographic filtering
- Google Sheets or Excel — basic distance calculations using the ACOS formula
- R or Python — statistical spatial analysis, cluster detection, regression modeling
Geocoding is the step that makes everything else possible. Without coordinates, patient data cannot touch census tables, HRSA designations, CDC surveillance data, or FEMA flood maps. With coordinates, every one of those datasets becomes joinable.
Geocoding Patient Data with the API
For organizations that need to geocode patient addresses in real time — at registration, not in monthly batches — the geocoding API returns coordinates on every request with 19 endpoints covering forward, reverse, and batch geocoding.
Single Address Lookup
curl "https://api.csv2geo.com/v1/geocode?q=350+Fifth+Avenue,+New+York,+NY+10118&country=US" \
-H "Authorization: Bearer YOUR_API_KEY"Response:
{
"results": [{
"formatted_address": "350 Fifth Avenue, New York, NY 10118, US",
"location": { "lat": 40.748817, "lng": -73.985428 },
"accuracy": "rooftop",
"accuracy_score": 1.0,
"components": {
"house_number": "350",
"street": "Fifth Avenue",
"city": "New York",
"state": "NY",
"postcode": "10118",
"country": "US"
}
}]
}Batch Geocoding (Up to 10,000 Addresses)
curl -X POST "https://api.csv2geo.com/v1/geocode" \
-H "Authorization: Bearer YOUR_API_KEY" \
-H "Content-Type: application/json" \
-d '{
"addresses": [
"742 Evergreen Terrace, Springfield, IL 62704",
"1600 Pennsylvania Ave NW, Washington, DC 20500",
"350 Fifth Avenue, New York, NY 10118"
]
}'The batch endpoint processes up to 10,000 addresses per request. For a hospital with 50,000 patient records, that is five API calls — completed in under a minute.
Python Example for EHR Integration
import csv
import requests
API_KEY = "your_api_key_here"
API_URL = "https://api.csv2geo.com/v1/geocode"
# Read patient addresses from EHR export
with open("patient_addresses.csv") as f:
reader = csv.DictReader(f)
addresses = [
f"{row['Street']}, {row['City']}, {row['State']} {row['ZIP']}"
for row in reader
]
# Batch geocode in chunks of 10,000
for i in range(0, len(addresses), 10000):
chunk = addresses[i:i+10000]
response = requests.post(API_URL, json={"addresses": chunk},
headers={"Authorization": f"Bearer {API_KEY}"})
results = response.json()["results"]
for result in results:
lat = result["location"]["lat"]
lng = result["location"]["lng"]
score = result["accuracy_score"]
print(f"{lat}, {lng} (confidence: {score})")HIPAA Compliance: Geocoding Patient Addresses Safely
Patient addresses are Protected Health Information (PHI) under HIPAA. Any geocoding workflow that processes patient addresses must comply with HIPAA’s Privacy Rule and Security Rule. Here is how to do it safely.
Is geocoding a patient address a HIPAA violation?
No. Geocoding is a data processing activity, not a disclosure. You are converting one form of the address (text) into another form (coordinates). As long as the geocoding service handles the data securely and does not retain, log, or share the addresses, it is no different from any other data processing operation under a Business Associate Agreement.
HIPAA-Safe Geocoding Checklist
| Requirement | What It Means | CSV2GEO |
|---|---|---|
| Data minimization | Only send the address — strip names, DOB, SSN, MRN before uploading | ✓ Only address columns needed |
| Encryption in transit | HTTPS/TLS for all data transmission | ✓ TLS 1.3 on all endpoints |
| No data retention | Addresses not stored after processing | ✓ Results deleted after download |
| No logging of PHI | Addresses not written to application logs | ✓ API supports no_record mode |
| Access controls | API keys, role-based access | ✓ Per-user API keys |
| BAA available | Business Associate Agreement for covered entities | ✓ Available on request |
Practical HIPAA Workflow
- Export patient addresses from your EHR into a CSV file. Include only the address fields (street, city, state, ZIP) and a non-PHI identifier (an internal ID number, not name or MRN).
- Geocode the addresses. Upload the stripped CSV to CSV2GEO or call the API. No names, no DOBs, no medical records.
- Download the geocoded file. The output adds latitude, longitude, and confidence score to each row.
- Join back to your patient records. Match on the internal ID to re-link coordinates with patient demographics inside your secure environment.
- Delete the intermediate files. The CSV you uploaded and downloaded should be deleted from your workstation once the coordinates are in your secure system.
This workflow ensures that PHI exposure is minimized. The geocoding service only ever sees addresses and internal IDs — not enough to identify any individual patient.
De-Identification Under HIPAA Safe Harbor
HIPAA’s Safe Harbor method for de-identification requires removing geographic data smaller than a state. However, this applies to de-identified datasets intended for research publication — not operational geocoding. Your internal analytics team can use full geocoded addresses as long as the data remains within your covered entity and business associates. The key distinction: geocoding for internal operations is permitted; publishing geocoded patient data is not (without proper de-identification).
Geocoding Options for Healthcare Organizations
| Feature | CSV2GEO | Google Maps API | US Census Geocoder | ArcGIS Geocoding |
|---|---|---|---|---|
| Batch upload (CSV) | ✓ Drag & drop | ✗ API only | ✓ 10,000 limit | ✓ With ArcGIS Pro |
| Free tier | 100 rows/day + 1,000 API/day | $200/month credit | Unlimited (US only) | 1,000/month |
| Coverage | 200+ countries (461M addresses) | Global | US only | Global |
| HIPAA-compatible | ✓ No-record mode, BAA | ⚠ BAA via Google Cloud | ✓ Government-operated | ⚠ BAA via Esri |
| Speed (10,000 rows) | ~15 seconds | ~5 minutes (rate limits) | ~10 minutes | ~2 minutes |
| API endpoints | 19 endpoints | 4 endpoints | 2 endpoints | 3 endpoints |
| No signup required | ✓ | ✗ | ✓ | ✗ |
| Confidence scores | ✓ 0.0–1.0 | ✗ Match type only | ⚠ Match/No match | ✓ 0–100 |
For healthcare organizations that need batch geocoding with HIPAA compliance and no per-lookup charges, CSV2GEO provides the most practical option. The US Census Geocoder is free and government-operated but limited to US addresses and significantly slower. Google Maps is accurate but expensive at scale and requires API development.
Real-World Healthcare Geocoding Examples
Example 1: FQHC Grant Reporting (HRSA UDS)
Federally Qualified Health Centers report patient demographics to HRSA annually through the Uniform Data System (UDS). UDS Table 3A requires reporting patients by ZIP code. But for HRSA’s New Access Point (NAP) grants, applicants must demonstrate that their proposed service area has a shortage of primary care providers — which requires geocoding patient addresses, mapping them against Health Professional Shortage Area (HPSA) boundaries, and calculating the percentage of patients living in underserved areas.
Workflow: Export 23,000 patient addresses → batch geocode → join with HRSA HPSA shapefile → calculate: 67% of patients live in a primary care HPSA → include this statistic in the NAP grant application.
Example 2: Hospital CHNA with Social Determinants
A non-profit hospital in Ohio conducts its triennial CHNA. They geocode 85,000 inpatient and outpatient addresses, join with American Community Survey data at the census tract level, and discover that patients from tracts with >25% poverty rates have 3.2x higher emergency department utilization. This finding drives the hospital’s community benefit spending toward a patient navigation program targeting those specific census tracts.
Example 3: Health Plan Network Adequacy Filing
A Medicare Advantage plan in Texas geocodes 180,000 member addresses and 12,000 contracted provider addresses. They run pairwise distance calculations and identify that 4,200 rural members in West Texas lack access to a cardiologist within 75 miles. The plan adds three telehealth cardiology contracts to close the gap before the CMS filing deadline.
Frequently Asked Questions
Is it safe to geocode patient addresses under HIPAA?
Yes, as long as you minimize the data sent (address only, no names or medical records), use encrypted connections (HTTPS), and work with a geocoding service that does not retain or log your data. A Business Associate Agreement adds formal protection. Geocoding is a data processing activity, not a disclosure.
How accurate is geocoding for healthcare applications?
CSV2GEO geocodes to rooftop accuracy (the exact building) for addresses in its 461 million record database. For patient access analysis, this means distance calculations are accurate to within meters, not miles. The confidence score on each result tells you exactly how precise the match is.
Can I geocode addresses from Epic or Cerner?
Yes. Export patient demographics as a CSV from any EHR system. Most systems have a standard report or data extract function. You only need address fields (street, city, state, ZIP) — exclude all clinical and identifying data before geocoding.
How many addresses can I geocode at once?
The batch geocoding file upload handles files up to 500,000 rows. The API supports 10,000 addresses per request with unlimited requests. Most hospital patient registries (10,000–200,000 records) process in under five minutes.
What about international patient addresses?
CSV2GEO covers 200+ countries with 461 million addresses. This is particularly relevant for organizations serving immigrant populations, military families stationed overseas, or global health programs operating across multiple countries.
Can I integrate geocoding into our EHR workflow?
Yes. The geocoding API integrates with any system that can make HTTP requests — EHR middleware, nightly batch jobs, analytics dashboards. It has 19 endpoints covering forward geocoding, reverse geocoding, batch processing, and place lookups.
What is the cost of geocoding for a hospital?
The free tier covers 100 rows per day (file upload) and 3,000 API requests per day — enough for small clinics and pilot projects. Subscriptions start at $49/month for 100,000 lookups. For context, geocoding 200,000 patient addresses costs $1,000 with Google Maps versus $29 with CSV2GEO. We break this down in the geocoding API pricing comparison.
Does the US Census Geocoder work for healthcare?
The US Census Geocoder is free and government-operated, which is appealing for HIPAA-sensitive work. However, it is limited to US addresses, processes slowly (10,000 records maximum per batch), and lacks confidence scores. For small one-time projects it works. For ongoing operational geocoding, a dedicated service is more practical.
Start Geocoding Your Patient Data
Upload your patient addresses to the free batch geocoding tool and get coordinates with confidence scores in minutes — 100 rows per day, no signup, no credit card. For EHR or analytics platform integration, grab a free API key from the geocoding API dashboard (1,000 requests/day included).
I.A. / CSV2GEO Creator
Related Articles
Use our batch geocoding tool to convert thousands of addresses to coordinates in minutes. Start with 100 free addresses.
Try Batch Geocoding Free →